- Chlamydia infection
-
For Chlamydia's life cycle, see Chlamydia (bacterium)For infectious agents previously designated Chlamydiae, see species of Chlamydophila
Chlamydia Classification and external resources 
Pap smear showing C. trachomatis (H&E stain)ICD-10 A55-A56.8, A70-A74.9 ICD-9 099.41, 483.1 DiseasesDB 2384 eMedicine med/340 MeSH D002690 Chlamydia infection (from the Greek, χλαμύδα meaning "cloak") is a common sexually transmitted infection (STI) in humans caused by the bacterium Chlamydia trachomatis. The term Chlamydia infection can also refer to infection caused by any species belonging to the bacterial family Chlamydiaceae. C. trachomatis is found only in humans.[1] Chlamydia is a major infectious cause of human genital and eye disease. Chlamydia infection is one of the most common sexually transmitted infections worldwide; it is estimated that about 1 million individuals in the United States are infected with chlamydia.[2]
C. trachomatis is naturally found living only inside human cells. Chlamydia can be transmitted during vaginal, anal, or oral sex, and can be passed from an infected mother to her baby during vaginal childbirth. Between half and three-quarters of all women who have a chlamydia infection of the neck of the womb (cervicitis) have no symptoms and do not know that they are infected. In men, infection of the urethra (urethritis) is usually symptomatic, causing a white discharge from the penis with or without pain on urinating (dysuria). Occasionally, the condition spreads to the upper genital tract in women (causing pelvic inflammatory disease) or to the epididymis in men (causing epididymitis). If untreated, chlamydial infections can cause serious reproductive and other health problems with both short-term and long-term consequences.
Chlamydia conjunctivitis or trachoma is a common cause of blindness worldwide. The World Health Organization (WHO) estimates that it accounted for 15% of blindness cases in 1995, but only 3.6% in 2002.[3][4][5]
Contents
Signs and symptoms
Genital disease
 Chlamydial cervicitis in a female patient characterized by mucopurulent cervical discharge, erythema, and inflammation.
Chlamydial cervicitis in a female patient characterized by mucopurulent cervical discharge, erythema, and inflammation.
 Male patients may develop a white, cloudy or watery discharge (shown) from the tip of the penis.
Male patients may develop a white, cloudy or watery discharge (shown) from the tip of the penis.
Women
Chlamydial infection of the neck of the womb (cervicitis) is a sexually transmitted infection which is asymptomatic for about 50-70% of women infected with the disease. The infection can be passed through vaginal, anal, or oral sex. Of those who have an asymptomatic infection that is not detected by their doctor, approximately half will develop pelvic inflammatory disease (PID), a generic term for infection of the uterus, fallopian tubes, and/or ovaries. PID can cause scarring inside the reproductive organs, which can later cause serious complications, including chronic pelvic pain, difficulty becoming pregnant, ectopic (tubal) pregnancy, and other dangerous complications of pregnancy.
Chlamydia is known as the "Silent Epidemic" because in women, it may not cause any symptoms in 75% of cases,[6] and can linger for months or years before being discovered. Symptoms that may occur include unusual vaginal bleeding or discharge, pain in the abdomen, painful sexual intercourse (dyspareunia), fever, painful urination or the urge to urinate more frequently than usual (urinary urgency).
Men
In men, chlamydia shows symptoms of infectious urethritis (inflammation of the urethra) in about 50% of cases.[6] Symptoms that may occur include: a painful or burning sensation when urinating, an unusual discharge from the penis, swollen or tender testicles, or fever. Discharge, or the purulent exudate, is generally less viscous and lighter in color than for gonorrhea. If left untreated, it is possible for chlamydia in men to spread to the testicles causing epididymitis, which in rare cases can cause sterility if not treated within 6 to 8 weeks. Chlamydia is also a potential cause of prostatitis in men, although the exact relevance in prostatitis is difficult to ascertain due to possible contamination from urethritis.[7]
Eye disease
Main article: TrachomaChlamydia conjunctivitis or trachoma was once the most important cause of blindness worldwide, but its role diminished from 15% of blindness cases by trachoma in 1995 to 3.6% in 2002.[3][4] The infection can be spread from eye to eye by fingers, shared towels or cloths, coughing and sneezing and eye-seeking flies.[8] Newborns can also develop chlamydia eye infection through childbirth (see below). Using the SAFE strategy (acronym for surgery for in-growing or in-turned lashes, antibiotics, facial cleanliness, and environmental improvements), the World Health Organisation aims for the global elimination of trachoma by 2020 (GET 2020 initiative).[9][10]
Rheumatological conditions
Chlamydia may also cause reactive arthritis (reiter's syndrome) - the triad of arthritis, conjunctivitis and urethritis (inflammation of the urethra) - especially in young men. About 15,000 men develop reactive arthritis due to chlamydia infection each year in the U.S., and about 5,000 are permanently affected by it. It can occur in both sexes, though is more common in men.
Perinatal infections
As many as half of all infants born to mothers with chlamydia will be born with the disease. Chlamydia can affect infants by causing spontaneous abortion; premature birth; conjunctivitis, which may lead to blindness; and pneumonia. Conjunctivitis due to chlamydia typically occurs one week after birth (compared with chemical causes (within hours) or gonorrhea (2–5 days)).
Other conditions
Chlamydia trachomatis is also the cause of lymphogranuloma venereum, an infection of the lymph nodes and lymphatics. It usually presents with genital ulceration and swollen lymph nodes in the groin, but it may also manifest as proctitis (inflammation of the rectum), fever or swollen lymph nodes in other regions of the body.[11]
Transmission
Chlamydia can be transmitted during vaginal, anal, or oral sex. Chlamydia can also be passed from an infected mother to her baby during vaginal childbirth.[12]
Pathophysiology
Chlamydiae have the ability to establish long-term associations with host cells. When an infected host cell is starved for various nutrients such as amino acids (for example, tryptophan),[13] iron, or vitamins, this has a negative consequence for Chlamydiae since the organism is dependent on the host cell for these nutrients. Long-term cohort studies indicate that approximately 50% of those infected clear within a year, 80% within two years, and 90% within three years.[14]
The starved chlamydiae enter a persistent growth state wherein they stop cell division and become morphologically aberrant by increasing in size.[15] Persistent organisms remain viable as they are capable of returning to a normal growth state once conditions in the host cell improve.
There is much debate as to whether persistence has in vivo relevance. Many believe that persistent chlamydiae are the cause of chronic chlamydial diseases. Some antibiotics such as β-lactams can also induce a persistent-like growth state, which can contribute to the chronicity of chlamydial diseases.
Screening
For sexually active women who are not pregnant, screening is recommended in those under 25 and others at risk of infection.[16] Risk factors include a history of chlamydial or other sexually transmitted infection, new or multiple sexual partners, and inconsistent condom use.[17] For pregnant women, guidelines vary: screening women with age or other risk factors is recommended by the U.S. Preventive Services Task Force (USPSTF) (which recommends screening women under 25) and the American Academy of Family Physicians (which recommends screening women aged 25 or younger). The American College of Obstetricians and Gynecologists recommends screening all at risk, while the Centers for Disease Control and Prevention recommend universal screening of pregnant women.[16] The USPSTF acknowledges that in some communities there may be other risk factors for infection, such as ethnicity.[16] Evidence-based recommendations for screening initiation, intervals and termination are currently not possible.[16] There is no universal agreement on screening men for chlamydia.[why?]
In England and Wales the NHS National Chlamydia Screening Programme (NCSP) aims to
- Prevent and control chlamydia infection through early detection and treatment of asymptomatic infection;
- Reduce onward transmission to sexual partners;
- Prevent the consequences of untreated infection;
- Test at least 25 percent of the sexually active under 25 population annually.[18]
Diagnosis
The diagnosis of genital chlamydial infections evolved rapidly from the 1990s through 2006. Nucleic acid amplification tests (NAAT), such as polymerase chain reaction (PCR), transcription mediated amplification (TMA), and the DNA strand displacement amplification (SDA) now are the mainstays. NAAT for chlamydia may be performed on swab specimens collected from the cervix (women) or urethra (men), on self-collected vaginal swabs, or on voided urine.[19] Urine and self-collected swab testing facilitates the performance of screening tests in settings where genital examination is impractical. At present, the NAATs have regulatory approval only for testing urogenital specimens, although rapidly evolving research indicates that they may give reliable results on rectal specimens.
Because of improved test accuracy, ease of specimen management, convenience in specimen management, and ease of screening sexually active men and women, the NAATs have largely replaced culture, the historic gold standard for chlamydia diagnosis, and the non-amplified probe tests. The latter test is relatively insensitive, successfully detecting only 60-80% of infections in asymptomatic women, and often giving falsely positive results. Culture remains useful in selected circumstances and is currently the only assay approved for testing non-genital specimens.
Treatment
C. trachomatis infection can be effectively cured with antibiotics once it is detected. Current guidelines recommend: azithromycin, doxycycline, erythromycin, or ofloxacin.[20] Agents recommended for pregnant women include erythromycin or amoxicillin.[21]
An option for treating partners of patients (index cases) diagnosed with chlamydia or gonorrhea is patient-delivered partner therapy (PDT or PDPT), which is the clinical practice of treating the sex partners of index cases by providing prescriptions or medications to the patient to take to his/her partner without the health care provider first examining the partner.[22]
Epidemiology
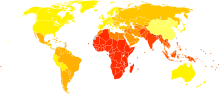 Age-standardized death from chlamydia per 100,000 inhabitants in 2004.[23]
Age-standardized death from chlamydia per 100,000 inhabitants in 2004.[23] no data≤1010-2020-3030-4040-5050-6060-7070-8080-9090-100100-110more than 110
no data≤1010-2020-3030-4040-5050-6060-7070-8080-9090-100100-110more than 110Chlamydia causes more than 250,000 cases of epididymitis in the U.S. each year. Chlamydia causes 250,000 to 500,000 cases of PID every year in the United States. Women infected with chlamydia are up to five times more likely to become infected with HIV, if exposed.[24]
Evolution
Recent phylogenetic studies have revealed that Chlamydia likely shares a common ancestor with cyanobacteria, the group containing the endosymbiont ancestor to the chloroplasts of modern plants, hence, Chlamydia retains unusual plant-like traits, both genetically and physiologically. In particular, the enzyme L,L-diaminopimelate aminotransferase, which is related to lysine production in plants, is also linked with the construction of chlamydia's cell wall. The genetic encoding for the enzymes is remarkably similar in plants, cyanobacteria, and Chlamydia, demonstrating a close common ancestry.[25] This unexpected discovery may help scientists develop new treatment avenues: if scientists could find a safe and effective inhibitor of L,L-diaminopimelate aminotransferase, they might have a highly effective and extremely specific new antibiotic against chlamydia.[citation needed]
References
- ^ "www.chlamydiae.com (professional) - Taxonomy diagram". http://www.chlamydiae.com/docs/Chlamydiales/diagram/taxondiag.htm. Retrieved 2007-10-27.
- ^ Chlamydia fact sheet from the Centers for Disease Control and Prevention
- ^ a b Thylefors B, Négrel AD, Pararajasegaram R, Dadzie KY (1995). "Global data on blindness". Bull World Health Organ 73 (1): 115–21. PMC 2486591. PMID 7704921. http://whqlibdoc.who.int/bulletin/1995/Vol73-No1/bulletin_1995_73(1)_115-121.pdf.
- ^ a b Resnikoff S, Pascolini D, Etya'ale D et al. (2004). "Global data on visual impairment in the year 2002". Bull World Health Organ 82 (11): 844–851. PMC 2623053. PMID 15640920. http://www.who.int/bulletin/volumes/82/11/en/844.pdf.
- ^ Belland R, Ojcius D, Byrne G (2004). "Chlamydia". Nat Rev Microbiol 2 (7): 530–1. doi:10.1038/nrmicro931. PMID 15248311.
- ^ a b "FreeTest.Me - About Chlamydia". http://freetest.me.uk/about-chlamydia. Retrieved 2008-12-15.
- ^ Wagenlehner FM, Naber KG, Weidner W (2006). "Chlamydial infections and prostatitis in men". BJU Int. 97 (4): 687–90. doi:10.1111/j.1464-410X.2006.06007.x. PMID 16536754. http://www.blackwell-synergy.com/openurl?genre=article&sid=nlm:pubmed&issn=1464-4096&date=2006&volume=97&issue=4&spage=687.
- ^ Mabey DC, Solomon AW, Foster A (2003). "Trachoma". Lancet 362 (9379): 223–9. doi:10.1016/S0140-6736(03)13914-1. PMID 12885486. http://linkinghub.elsevier.com/retrieve/pii/S0140-6736(03)13914-1.
- ^ World Health Organisation. Trachoma. Accessed March 17, 2008.
- ^ Ngondi J, Onsarigo A, Matthews F, et al. (2006). "Effect of 3 years of SAFE (surgery, antibiotics, facial cleanliness, and environmental change) strategy for trachoma control in southern Sudan: a cross-sectional study". Lancet 368 (9535): 589–95. doi:10.1016/S0140-6736(06)69202-7. PMID 16905023. http://linkinghub.elsevier.com/retrieve/pii/S0140-6736(06)69202-7.
- ^ Williams D, Churchill D (2006). "Ulcerative proctitis in men who have sex with men: an emerging outbreak". BMJ 332 (7533): 99–100. doi:10.1136/bmj.332.7533.99. PMC 1326936. PMID 16410585. http://bmj.com/cgi/pmidlookup?view=long&pmid=16410585.
- ^ http://www.cdc.gov/std/chlamydia/stdfact-chlamydia.htm
- ^ Leonhardt RM, Lee SJ, Kavathas PB, Cresswell P (2007). "Severe Tryptophan Starvation Blocks Onset of Conventional Persistence and Reduces Reactivation of Chlamydia trachomatis". Infect. Immun. 75 (11): 5105–17. doi:10.1128/IAI.00668-07. PMC 2168275. PMID 17724071. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2168275.
- ^ Fairley et al., CK; Gurrin, L; Walker, J; Hocking, JS (2007). ""Doctor, How Long Has My Chlamydia Been There?" Answer:"... Years"". Sexually Transmitted Diseases 34 (9): 727. doi:10.1097/OLQ.0b013e31812dfb6e. PMID 17717486. http://www.stdjournal.com/pt/re/std/fulltext.00007435-200709000-00018.htm.
- ^ Mpiga P, Ravaoarinoro M (2006). "Chlamydia trachomatis persistence: an update". Microbiol. Res. 161 (1): 9–19. doi:10.1016/j.micres.2005.04.004. PMID 16338585.
- ^ a b c d Meyers D, Wolff T, Gregory K. et al. USPSTF Recommendations for STI Screening. Am Fam Physician. 2008;77(6):819-824.
- ^ U.S. Preventive Services Task Force (2007). "Screening for chlamydial infection: U.S. Preventive Services Task Force recommendation statement". Ann Intern Med 147 (2): 128–34. PMID 17576996. http://www.ahrq.gov/clinic/uspstf07/chlamydia/chlamydiars.htm.
- ^ "National Chlamydia Screening Programme Data tables". http://www.chlamydiascreening.nhs.uk/ps/data/data_tables.html. Retrieved 2009-08-28.
- ^ Gaydos CA et al (2004). Comparison of three nucleic acid amplification tests for detection of Chlamydia trachomatis in urine specimens. J Clin Microbio 42(7):3041-3045. DOI: 10.1128/JCM.42.7.3041-3045.2004
- ^ al.], David N. Gilbert ... [et. The Sanford guide to antimicrobial therapy 2011. Sperryville, VA: Antimicrobial Therapy, Inc.. pp. 20. ISBN 1930808658.
- ^ "Diagnosis and Treatment of Chlamydia trachomatis Infection - April 15, 2006 - American Family Physician". http://www.aafp.org/afp/2006/0415/p1411.html. Retrieved 2010-10-30.
- ^ Expedited Partner Therapy in the Management of Sexually Transmitted Diseases (2 February 2006) U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES PUBLIC HEALTH SERVICE. Centers for Disease Control and Prevention National Center for HIV, STD, and TB Prevention
- ^ "WHO Disease and injury country estimates". World Health Organization. 2004. http://www.who.int/healthinfo/global_burden_disease/estimates_country/en/index.html. Retrieved Nov. 11, 2009.
- ^ "STD Facts - Chlamydia". http://www.cdc.gov/std/chlamydia/STDFact-Chlamydia.htm#complications. Retrieved 2007-10-26.
- ^ McCoy AJ, Adams NE, Hudson AO, Gilvarg C, Leustek T, Maurelli AT (2006). "L,L-diaminopimelate aminotransferase, a trans-kingdom enzyme shared by Chlamydia and plants for synthesis of diaminopimelate/lysine". Proc. Natl. Acad. Sci. U.S.A. 103 (47): 17909–14. doi:10.1073/pnas.0608643103. PMC 1693846. PMID 17093042. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=1693846.
External links
- Chlamydia Fact Sheet from the CDC
- Links to chlamydia pictures at University of Iowa
- Chlamydiae.com includes some information in multiple languages
- The National Chlamydia Screening Programme – The NCSP's official website containing information.
- Freetest.me – National free postal testing service operating across England.
Sexually transmitted diseases and infections (STD/STI) (primarily A50–A64, 090–099) Bacterial Chancroid (Haemophilus ducreyi) · Chlamydia/Lymphogranuloma venereum (Chlamydia trachomatis) · Donovanosis or Granuloma Inguinale (Klebsiella granulomatis) · Gonorrhea (Neisseria gonorrhoeae) · Syphilis (Treponema pallidum) · Ureaplasma infection (Ureaplasma urealyticum)Protozoal Parasitic Viral AIDS (HIV-1/HIV-2) · Cervical cancer, vulvar cancer & Genital warts (condyloma), Penile cancer, Anal cancer (Human papillomavirus (HPV)) · Hepatitis B (Hepatitis B virus) · Herpes simplex (HSV1/HSV2) · Molluscum contagiosum (MCV)General
inflammationCategories:- Sexually transmitted diseases and infections
- Bacterial diseases
- Chlamydiae
Wikimedia Foundation. 2010.


