- Liquid breathing
-
Liquid breathing Intervention MeSH D021061 Liquid breathing is a form of respiration in which a normally air-breathing organism breathes an oxygen-rich liquid (such as a perfluorocarbon), rather than breathing air.
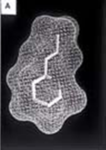
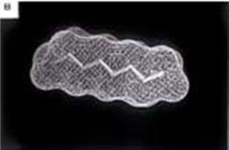
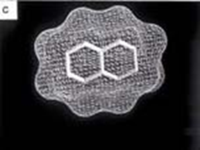
Computer models of three perfluorochemical molecules used for biomedical applications and for liquid ventilation studies: a) FC-75, b) perflubron, and c) perfluorodecalin.Perfluorochemical (perfluorocarbon) molecules have very different structures that impart different physical properties such as respiratory gas solubility, density, viscosity, vapor pressure, and lipid solubility.[1] Thus, it is critical to select the appropriate PFC for a specific biomedical application, such as liquid ventilation, drug delivery, blood substitutes, etc. The physical properties of PFC liquids vary substantially; however, the one common property is their high solubility for respiratory gases. In fact, these liquids carry more oxygen and carbon dioxide than blood.[2]
In theory, liquid breathing could assist in the treatment of patients with severe pulmonary or cardiac trauma, especially in pediatric cases. Liquid breathing has also been proposed for use in deep diving[3][4] and space travel.[5] Despite some recent advances in liquid ventilation, a standard mode of application has not been established yet.
Liquid breathing is sometimes called "fluid breathing", but this can be misleading, as normal atmospheric air is also a fluid.
Physicochemical properties (37°C at 1 atm) of 18 perfluorochemical liquids used for biomedical applications. This table characterizes the most significant physical properties related to systemic physiology and their range of properties. gas solubility Oxygen 33-66 mL / 100 mL PFC Carbon dioxide 140-166 mL / 100 mL PFC vapor pressure 0.2-400 torr density 1.58-2.0 g/mL viscosity 0.8-8.0 cS Contents
Approaches
Because liquid breathing is still a highly experimental technique, there are several proposed approaches.
Total liquid ventilation
Although total liquid ventilation (TLV) with completely liquid-filled lungs can be beneficial,[6] the complex liquid-filled tube system required is a disadvantage compared to gas ventilation - the system must incorporate a membrane oxygenator, heater, and pumps to deliver to, and remove from the lungs tidal volume aliquots of conditioned perfluorocarbon (PFC). One research group led by Thomas H. Shaffer has maintained that with the use of microprocessors and new technology, it is possible to maintain better control of respiratory variables such as liquid functional residual capacity and tidal volume during TLV, than with gas ventilation.[1][7][8][9] Consequently, the total liquid ventilation necessitates a dedicated liquid ventilator similar to a medical ventilator except that it uses a breatheable liquid. Many prototypes are used for animal experimentations, but experts recommend continued development of a liquid ventilator toward clinical applications.[10]
Partial liquid ventilation
In contrast, partial liquid ventilation (PLV) is a technique in which a PFC is instilled into the lung to a volume approximating functional residual capacity (approximately 40% of Total Lung Capacity (TLC)). Conventional mechanical ventilation delivers tidal volume breaths on top of it. This mode of liquid ventilation currently seems technologically more feasible than total liquid ventilation, because PLV could utilise technology currently in place in many neonatal intensive-care units (NICU) worldwide.
The influence of PLV on oxygenation, carbon dioxide removal and lung mechanics has been investigated in several animal studies using different models of lung injury[11] Clinical applications of PLV have been reported in patients with acute respiratory distress syndrome (ARDS), meconium aspiration syndrome, congenital diaphragmatic hernia and respiratory distress syndrome (RDS) of neonates. In order to correctly and effectively conduct PLV, it is essential to
- properly dose a patient to a specific lung volume (10-15 ml/kg) to recruit alveolar volume and
- redose the lung with PFC liquid (1-2 ml/kg/hr) to oppose PFC evaporation from the lung.
If PFC liquid is not maintained in the lung, PLV can not effectively protect the lung from biophysical forces associated with the gas ventilator.
New application modes for PFC have been developed.[12]
PFC vapor
Vaporization of perfluorohexane with two anesthetic vaporizers calibrated for perfluorohexane has been shown to improve gas exchange in oleic acid-induced lung injury in sheep.[13]
Predominantly PFCs with high vapor pressure are suitable for vaporization
Aerosol-PFC
With aerosolized perfluorooctane, significant improvement of oxygenation and pulmonary mechanics was shown in adult sheep with oleic acid-induced lung injury.
In surfactant-depleted piglets, persistent improvement of gas exchange and lung mechanics was demonstrated with Aerosol-PFC.[14] The aerosol device is of decisive importance for the efficacy of PFC aerosolization, as aerosolization of PF5080 (a less purified FC77) has been shown to be ineffective using a different aerosol device in surfactant-depleted rabbits. Partial liquid ventilation and Aerosol-PFC reduced pulmonary inflammatory response.[15]
Proposed uses
Diving
Gas pressure increases with depth, rising 1 bar every 10 meters to over 1,000 bar at the bottom of the Mariana Trench. Diving becomes more dangerous as depth increases, and deep diving presents many hazards. All surface-breathing animals are subject to decompression sickness, including aquatic mammals[16] and free-diving humans (see taravana). Breathing at depth can cause nitrogen narcosis and oxygen toxicity. Ascending after breathing at depth can cause air embolisms, burst lung, and collapsed lung.
Special breathing gas mixes such as trimix or heliox ameliorate the risk of decompression illness but do not eliminate it. Heliox further eliminates the risk of nitrogen narcosis but introduces the risk of helium tremors below 500 feet (152 meters). Atmospheric diving suits maintain body and breathing pressure at 1 bar, eliminating most of the hazards of descending, ascending, and breathing at depth. However, the rigid suits are bulky, clumsy, and very expensive.
Liquid breathing offers a third option,[3][17] promising the mobility available with flexible dive suits and the reduced risks of rigid suits. With liquid in the lungs, the pressure within the diver's lungs could accommodate changes in the pressure of the surrounding water without the huge gas partial pressure exposures required when the lungs are filled with gas. Liquid breathing would not result in the saturation of body tissues with high pressure nitrogen or helium that occurs with the use of non-liquids, thus would reduce or remove the need for slow decompression.
A significant problem, however, arises from the high viscosity of the liquid and the corresponding reduction in its ability to remove CO2.[3][18] All uses of liquid breathing for diving must involve total liquid ventilation (see above). Total liquid ventilation, however, has difficulty moving enough liquid to carry away CO2, because no matter how great the total pressure is, the amount of partial CO2 gas pressure available to dissolve CO2 into the breathing liquid can never be much more than the pressure at which CO2 exists in the blood (about 40 mm of mercury (Torr)).[18]
At these pressures, most fluorocarbon liquids require about 70 mL/kg minute-ventilation volumes of liquid (about 5 L/min for a 70 kg adult) to remove enough CO2 for normal resting metabolism.[19] This is a great deal of fluid to move, particularly as liquids are generally more viscous than gases, (for example water is about 850 times the viscosity of air[20]). Any increase in the diver's metabolic activity also increases CO2 production and the breathing rate, which is already at the limits of realistic flow rates in liquid breathing.[3][21][22] It seems unlikely that a person would move 10 liters/min of fluorocarbon liquid without assistance from a mechanical ventilator, so "free breathing" may be unlikely.
Medical treatment
The most promising area for the use of liquid ventilation is in the field of pediatric medicine.[23][24][25] The first medical use of liquid breathing was treatment of premature babies[26][27][28][29] and adults with acute respiratory distress syndrome (ARDS) in the 1990s. Liquid breathing was used in clinical trials after the development by Alliance Pharmaceuticals of the fluorochemical perfluorooctyl bromide, or perflubron for short. Current methods of positive-pressure ventilation can contribute to the development of lung disease in pre-term neonates, leading to diseases such as bronchopulmonary dysplasia. Liquid ventilation removes many of the high pressure gradients responsible for this damage. Furthermore, perfluorocarbons have been demonstrated to reduce lung inflammation,[30][31][32] improve ventilation-perfusion mismatch and to provide a novel route for the pulmonary administration of drugs.[33][34][35]
In order to explore drug delivery techniques that would be useful for both partial and total liquid ventilation, more recent studies have focused on PFC drug delivery using a nanocrystal suspension. The first image is a computer model of a PFC liquid (perflubron) combined with gentamicin molecules.
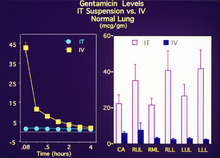
The second image shows experimental results comparing both plasma and tissue levels of gentamicin after an intratracheal (IT) and intravenous (IV) dose of 5 mg/kg in a newborn lamb during gas ventilation. Note that the plasma levels of the IV dose greatly exceed the levels of the IT dose over the 4 hour study period; whereas, the lung tissue levels of gentamicin when delivered by an intratracheal (IT) suspension, uniformly exceed the intravenous (IV) delivery approach after 4 hours. Thus, the IT approach allows more effective delivery of the drug to the target organ while maintaining a safer level systemically. Both images represent the in-vivo time course over 4 hours. Numerous studies have now demonstrated the effectiveness of PFC liquids as a delivery vehicle to the lungs.[36][37][38][39][40][41][42][43][44][45]
Clinical trials with premature infants, children and adults were conducted. Since the safety of the procedure and the effectiveness were apparent from an early stage, the US Food and Drug Administration (FDA) gave the product "fast track" status (meaning an accelerated review of the product, designed to get it to the public as quickly as is safely possible) due to its life-saving potential. Clinical trials showed that using perflubron with ordinary ventilators improved outcomes as much as using high frequency oscillating ventilation (HFOV). But because perflubron was not better than HFOV, the FDA did not approve perflubron, and Alliance is no longer pursuing the partial liquid ventilation application. Whether perflubron would improve outcomes when used with HFOV remains an open question.
In 1996 Mike Darwin and Dr. Steven B. Harris proposed using cold liquid ventilation with perfluorocarbon to quickly lower the body temperature of victims of cardiac arrest and other brain trauma to allow the brain to better recover.[46] The technology came to be called gas/liquid ventilation (GLV), and was shown able to achieve a cooling rate of 0.5° C per minute in large animals.[47] It has not yet been tried in humans.
Most recently, hypothermic brain protection has been associated with rapid brain cooling. In this regard, a new therapeutic approach is the use of intranasal perfluorochemical spray for preferential brain cooling.[48] The nasopharyngeal (NP) approach is unique for brain cooling due to anatomic proximity to the cerebral circulation and arteries. Based on preclinical studies in adult sheep, it was shown that independent of region, brain cooling was faster during NP-perfluorochemical versus conventional whole body cooling with cooling blankets. To date, there have been four human studies including a completed randomized intra-arrest study (200 patients).[49][50] Results clearly demonstrated that prehospital intra-arrest transnasal cooling is safe, feasible and is associated with an improvement in cooling time.
Space travel
Liquid immersion provides a way to reduce the physical stress of G forces. Forces applied to fluids are distributed as omnidirectional pressures. Because liquids cannot be practically compressed, they do not change density under high acceleration such as performed in aerial maneuvers or space travel. A person immersed in liquid of the same density as tissue has acceleration forces distributed around the body, rather than applied at a single point such as a seat or harness straps. This principle is used in a new type of G-suit called the Libelle G-suit, which allows aircraft pilots to remain conscious and functioning at more than 10 G acceleration by surrounding them with water in a rigid suit.
Acceleration protection by liquid immersion is limited by the differential density of body tissues and immersion fluid, limiting the utility of this method to about 15 to 20 G.[51] Extending acceleration protection beyond 20 G requires filling the lungs with fluid of density similar to water. An astronaut totally immersed in liquid, with liquid inside all body cavities, will feel little effect from extreme G forces because the forces on a liquid are distributed equally, and in all directions simultaneously. However effects will be felt because of density differences between different body tissues, so an upper acceleration limit still exists.
Liquid breathing for acceleration protection may never be practical because of the difficulty of finding a suitable breathing medium of similar density to water that is compatible with lung tissue. Perfluorocarbon fluids are twice as dense as water, hence unsuitable for this application.[2] On the other hand, although perfluorochemicals are denser than water, lung tissue floats within the PFC filled lungs, and if the lungs are not over-filled, there is no compromise in pulmonary or systemic blood flow.[52] Therefore, if the astronaut is immersed in liquid and their lungs are filled with liquid PFC, they should not experience adverse effects, in spite of the almost twofold density difference. Based on interviews with adult patients that experienced partial liquid ventilation, when they became conscious they were unaware that 20-30 ml/kg of PFC was in their lungs during recovery.
Examples in fiction
- Joe Haldeman's 1975 Novel The Forever War describes liquid immersion and breathing in great detail as a key technology to allow space travel and combat with acceleration up to 25 G.
- In The Lost Symbol by Dan Brown, Robert Langdon (the protagonist) is completely submerged in breathable liquid mixed with hallucination agents and sedatives as a torture technique by Mal'akh (the antagonist). He goes through a near death experience when he inhales the liquid and blacks out, losing control over his body, but is soon revived.
- The James Cameron film The Abyss features a character using liquid breathing to dive thousands of feet without compressing. The Abyss also features a scene with a rat submerged in and breathing fluorocarbon liquid, filmed in real life.[53]
- In the anime Neon Genesis Evangelion, the cockpits of the titular Mecha are filled with a fictional oxygenated liquid called LCL which helps to dampen impacts on the pilot in battle and helps him to better psychically-synchronize with his biomechanical vehicle.
- The aliens in the Gerry Anderson UFO series use liquid-breathing spacesuits.
- Hal Clement's 1973 novel Ocean on Top portrays a small underwater civilization living in a 'bubble' of oxygenated fluid denser than seawater.
- In an episode of the Adult Swim cartoon series Metalocalypse, the other members of the band submerge guitarist Toki in a "liquid oxygen isolation chamber" while recording an album in the Mariana Trench.
- In an episode of the SyFy Channel show Eureka, Sheriff Jack Carter is submerged in a tank of "oxygen rich plasma" to be cured of the effects of a scientific accident.
- In the movies Mission to Mars and Event Horizon, a character is depicted as being immersed in apparent breathable fluid before a high-acceleration launch.
- In season 1, episode 13 of Seven Days chrononaut Frank Parker is seen breathing a hyper-oxygenated perfluorocarbon liquid that is pumped through a sealed full body suit that he is wearing. This suit and liquid combination allow him to board a Russian submarine through open ocean at a depth of almost 1000 feet. Upon boarding the submarine he removes his helmet, expels the liquid from his lungs and is able to breathe air again.
- Ben Bova's novel Jupiter features a craft in which the crew are suspended in a breathable liquid that allows them to survive in the high pressure environment of Jupiter's atmosphere.
- In the book Mechanicum from the Horus Heresy series of novels in the Warhammer 40,000 setting, physically crippled Titan pilots are encased in nutrient fluid tanks to allow them to continue operating beyond the limits normally imposed by the body.
- In the classic PC Turn-Based Strategy game X-COM: Terror from the Deep, "Aquanauts" fighting deep ocean conditions breathe a dense oxygen-carrying fluid.
- In the Star Trek: The Next Generation novel "The Children of Hamlin" the crew of the Enterprise-D encounter an alien race whose ships contain a breathable liquid environment.
See also
- Mechanical ventilation
- Breathing gas
- Artificial gills (human)
- Liquid ventilator
References
- ^ a b Shaffer, T.H., M.R. Wolfson, and L.C. Clark: State of art review : Liquid ventilation. Pediatr. Pulmonol. 14:102 109, 1992
- ^ a b Gabriel et al. Quantitative structure-activity relationships of perfluorinated hetro-hydrocarbons as potential respiratory media. Application to oxygen solubility, partition coefficient, viscosity, vapor pressure, and density. ASAIO J. 42(6): 968-73, 1996.
- ^ a b c d Kylstra JA (1977). The Feasibility of Liquid Breathing in Man.. Report to the US Office of Naval Research. Durham, NC: Duke University. http://archive.rubicon-foundation.org/4257. Retrieved 2008-05-05.
- ^ "menfish". http://davidszondy.com/future/underwater/menfish.htm. Retrieved 2008-05-17.
- ^ "Liquid Breathing - Medical uses". http://www.experiencefestival.com/a/Liquid_breathing_-_Medical_uses/id/1580110. Retrieved 2008-05-17.
- ^ Wolfson et al. Multicenter comparative study of conventional mechanical gas ventilation to tidal liquid ventilation in oleic acid injured sheep 54(3):236-269, 2008.
- ^ Cox CA, Stavis RL. Wolfson MR, Shaffer TH: Long-term tidal liquid ventilation in premature lambs: Physiologic, biochemical and histological correlates. Biol. Neonate 84:232-242, 2003.
- ^ Libros R, CM Philips, MR Wolfson, and TH Shaffer: A perfluorochemical loss/restoration (L/R) system for tidal liquid ventilation. Biomed Instrum & Technol. 34(5): 351-360, 2000.
- ^ Heckman, JL, J Hoffman, TH Shaffer, and MR Wolfson: Software for real-time control of a tidal liquid ventilator. Biomedical Instrumentation & Technology 33(3):268-276, 1999.
- ^ Maria Laura Costantino, Philippe Micheau, Thomas H. Shaffer, Stefano Tredici, Maria R. Wolfson (2009). "Clinical Design Functions: Round table discussions on bioengineering of liquid ventilators". Asaio J. 55 (3): 206–8. doi:10.1097/MAT.0b013e318199c167. PMID 19282746. http://journals.lww.com/asaiojournal/Abstract/2009/05000/Clinical_Design_Functions__Round_Table_Discussions.4.aspx.
- ^ Clark, Leland C.; Gollan, F. (1966). "Survival of mammals breathing organic liquids equilibrated with oxygen at atmospheric pressure". Science 152 (3730): 1755–6. doi:10.1126/science.152.3730.1755. PMID 5938414.
- ^ "A significant positive step was the use of PFC-associated gas exchange, now termed partial liquid ventilation (PLV)." Hlastala, Michael P. and Jennifer E. Souders (July 1, 2001). "Perfluorocarbon Enhanced Gas Exchange". American Journal of Respiratory and Critical Care Medicine 164 (1): 1–2. PMID 11435228. http://ajrccm.atsjournals.org/cgi/content/full/164/1/1/.
- ^ "Vaporization is a new application technique for perfluorocarbon that significantly improved oxygenation and pulmonary function in oleic acid-induced lung injury." Bleyl JU et al. (1999). "Vaporized perfluorocarbon improves oxygenation and pulmonary function in an ovine model of acute respiratory distress syndrome". Anesthesiology 91 (2): 340–2. doi:10.1097/00000542-199908000-00021. PMID 10443610.
- ^ "Aerosolized perfluorocarbon improved pulmonary gas exchange and lung mechanics as effectively as PLV did in surfactant-depleted piglets, and the improvement was sustained longer." Kandler, Michael A. et al. (July 1, 2001). "Persistent Improvement of Gas Exchange and Lung Mechanics by Aerosolized Perfluorocarbon". American Journal of Respiratory and Critical Care Medicine 164 (1): 31–35. PMID 11435235. http://ajrccm.atsjournals.org/cgi/content/abstract/164/1/31?maxtoshow=&HITS=10&hits=10&RESULTFORMAT=&titleabstract=Aerosolized+Perfluorocarbon&searchid=1139153703244_1865&FIRSTINDEX=0&journalcode=ajrccm.
- ^ "In a surfactant-depleted piglet model, aerosol therapy with perfluorocarbon but not LV-PLV reduces the initial pulmonary inflammatory reaction at least as potently as PLV at FRC volume." von der Hardt, Katharina et al. (2002). "Aerosolized Perfluorocarbon Suppresses Early Pulmonary Inflammatory Response in a Surfactant-Depleted Piglet Model". Pediatric Research 51 (2): 177–182. doi:10.1203/00006450-200202000-00009. PMID 11809911. http://www.pedresearch.org/cgi/content/full/51/2/177/.
- ^ Lippsett, Lonny (5 April 2005). "Even Sperm Whales Get the Bends". Oceanus (Woods Hole Oceanographic Institution) 44 (1). Archived from the original on 3 August 2010. http://www.webcitation.org/5riSCNFYt. Retrieved 3 August 2010.
- ^ Kylstra JA (September 1974). "Liquid breathing". Undersea Biomed Res 1 (3): 259–69. PMID 4619862. http://archive.rubicon-foundation.org/2665. Retrieved 2008-05-05.
- ^ a b Matthews WH, Kylstra JA (June 1976). "A fluorocarbon emulsion with a high solubility for CO2". Undersea Biomed Res 3 (2): 113–20. PMID 951821. http://archive.rubicon-foundation.org/2764. Retrieved 2008-05-05.
- ^ Miyamoto Y., Mikami T. (1976). "Maximum capacity of ventilation and efficiency of gas exchange during liquid breathing in guinea pigs". Jpn. J. Physiol 26 (6): 603–618. doi:10.2170/jjphysiol.26.603. PMID 1030748.
- ^ Sherwood, Lauralee; Klandorf, Hillar; Yancey, Paul H. (2005). Animal Physiology: From Genes to Organisms. Southbank, Victoria, Australia: Thomson/Brooks/Cole. ISBN 0534554040. OCLC 224468651.
- ^ Koen, P. A.; Wolfson, M. R.; Shaffer, T. H. (1988). "Fluorocarbon ventilation: maximal expiratory flows and CO2 elimination". Pediatr Res. 24: 291–296. PMID 3145482
- ^ Matthews WH, Balzer RH, Shelburne JD, Pratt PC, Kylstra JA (December 1978). "Steady-state gas exchange in normothermic, anesthetized, liquid-ventilated dogs". Undersea Biomed Res 5 (4): 341–54. PMID 153624. http://archive.rubicon-foundation.org/2818. Retrieved 2008-05-05.
- ^ Wolfson et al. Perfluorochemical rescue after surfactant treatment: Effect of perflubron dose and ventilatory frequency J Appl Physiol. 84(2):624-40, 1998
- ^ Stavis et al. Physiologic, biochemical and histologic correlates associated with tidal liquid ventilation Pediatr Res 43(1):132-8, 1998
- ^ Wolfson MR and Shaffer TH Pulmonary applications of perfluorochemical liquids: Ventilation and beyond Paediatr Respir Rev 6(2): 117-27, 2005
- ^ Greenspan et al. Liquid ventilation of preterm baby. Lancet 2(8671): 1095, 1989.
- ^ Greenspan et al. Liquid ventilation of human neonates. J Pediatr. 117(1): 106-11, 1990.
- ^ Leach et al. Partial liquid ventilation with perflubron in premature infants with severe respiratory distress: The LiquiVent Study Group. N Engl J Med. 12; 335(11): 761-7, 1996.
- ^ Greenspan et al. Partial liquid ventilation in critically ill infants receiving extracorporeal life support. Philadelphia Liquid Ventilation Consortium Pediatrics 99(1): E2, 1997.
- ^ Brunelli et al. Perfluorochemical liquids enhance delivery of superoxide dismutase to the lungs of juvenile rabbits Pediatr Res 60(1):65-70, 2006.
- ^ Perfluorochemical liquids modulate cell-mediated inflammatory responses Crit Care Med. 29(9): 1731-7, 2001.
- ^ Babu et al. Hyperoxia -induced changes in human airway epithelial cells: The protective effect of perflubron. Pediatr Crit Care Med. 6(2): 188-94, 2005.
- ^ Brunelli et al.
- ^ Cox et al. Intra-tracheal administration of perfluorochemical-gentamicin suspension: A comparison to intravenous administration in normal and injured lungs. Pediatr Pulmonol. 32(2): 142-51, 2001.
- ^ Fox et al. Pulmonary administration of gentamicin during liquid ventilation in a newborn lamb lung injury model. Pediatrics 100(5): E5, 1997.
- ^ Wolfson MR, Greenspan JS, Shaffer TH. Pulmonary adminis¬tration of vasoactive substances by perfluorochemical ventilation. Pediatrics. 1996;97(4):449-455.
- ^ Kimless Garber DB, Wolfson MR, Carlsson C, Shaffer TH. Halothane administration during liquid ventila¬tion. Respir Med. 1997;91(5):255-262.
- ^ Zelinka MA, Wolfson MR, Calligaro I, Rubenstein SD, Greenspan JS, Shaffer TH. A comparison of intratracheal and intravenous administration of gentamicin during liquid ventilation. Eur J Pediatr. 1997;156(5):401-404.
- ^ Lisby DA, Ballard PL, Fox WW, Wolfson MR, Shaffer TH, Gonzales LW. Enhanced distribution of adenovirus-mediated gene transfer to lung parenchyma by perfluorochemical liquid. Hum Gene Ther. 1997;8(8):919-928.
- ^ Fox WW, Weis CM, Cox C, Farina C, Drott H, Wolfson MR, Shaffer TH. Pulmonary administration of gentamicin during liquid ventilation in a newborn lamb lung injury model. Pediatrics. 1997;100(5):E5.
- ^ Cullen AB, Cox CA, Hipp SJ, Wolfson MR, Shaffer TH. Intra-tracheal delivery strategy of gentamicin with partial liquid ventilation. Respir Med. 1999;93(11):770-778.
- ^ Cox CA, Cullen AB, Wolfson MR, Shaffer TH. Intratracheal administration of perfluorochemical-gentamicin suspension: a comparison to intravenous administration in normal and injured lungs. Pediatr Pulmonol. 2001;32(2):142-151.
- ^ Chappell SE, Wolfson MR, Shaffer TH. A comparison of surfactant delivery with conventional mechanical ventilation and partial liquid ventilation in meconium aspiration injury. Respir Med. 2001;95(7):612-617.
- ^ Brunelli L, Hamilton E, Davis JM, Koo HC, Joseph A, Kazzaz JA, Wolfson MR, Shaffer TH. Perfluorochemical liquids enhance delivery of superoxide dismutase to the lungs of juvenile rabbits. Pediatr Res. 2006;60(1):65-70.
- ^ Constantino ML, Shaffer TH, Wauer RR, Rudiger M. The 5th European Symposium on Perfluorocarbon (PFC) Application. ASAIO J. 2006;52(4):483-494.
- ^ Darwin, M.G. (1996). "Liquid Ventilation: A Bypass on The Way to Bypass". BPI Tech Briefs 19. http://www.cryocare.org/index.cgi?subdir=bpi&url=tech19.txt.
- ^ Harris, S.B. et al. (2001). "Rapid (0.5°C/min) minimally invasive induction of hypothermia using cold perfluorochemical lung lavage in dogs". Resusciation 50 (2): 189–204. doi:10.1016/S0300-9572(01)00333-1. PMID 11719148.
- ^ Wolfson et al. Intranasal perfluorochemical spray for preferential brain cooling in sheep. Neurocrit Care. 8(3): 437-47, 2008
- ^ Castrén M, Nordberg P, Svensson L, et al. Intra-arrest transnasal evaporative cooling: a randomized, prehospital, multicenter study (PRINCE: Pre-ROSC IntraNasal Cooling Effectiveness). Circulation. 2010 Aug 17;122(7):729-36. Epub 2010 Aug 2.
- ^ Busch HJ, Eichwede F, Födisch M, et al. Safety and feasibility of nasopharyngeal evaporative cooling in the emergency department setting in survivors of cardiac arrest. Resuscitation. 2010 Aug;81(8):943-9. Epub 2010 Jun 2.
- ^ Guyton, Arthur C. (1986). Textbook of Medical Physiology, 7th Ed., Aviation, Space, and Deep Sea Diving Physiology. W.B. Saunders Company. p. 533.
- ^ Davidson et al. Cardiopulmonary interaction during partial liquid ventilation in surfactant treated preterm lambs. Eur J. Pediatr. 157(2): 138-45, 1998.
- ^ ALJEAN HARMETZ; FILM; 'The Abyss': A Foray Into Deep Waters - The New York Times
External links
- Here, Breathe This Liquid from Discover Magazine
- Miracle Girl from Readers Digest
Wikimedia Foundation. 2010.