- Erythromelalgia
-
Erythromelalgia Classification and external resources 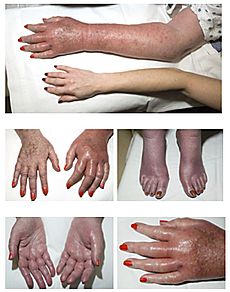
Erythromelalgia in a 77-year-old woman with longstanding polycythemia vera.ICD-10 I73.8 ICD-9 443.82 OMIM 133020 DiseasesDB 4476 eMedicine med/730 MeSH D004916 Erythromelalgia, also known as Mitchell's disease (after Silas Weir Mitchell), acromelalgia, red neuralgia, or erythermalgia,[1] is a rare neurovascular peripheral pain disorder in which blood vessels, usually in the lower extremities (or hands), are episodically blocked (frequently on and off daily), then become hyperemic and inflamed. There is severe burning pain (in the small fiber sensory nerves) and skin redness. The attacks are periodic and are commonly triggered by heat, pressure, mild activity, exertion, insomnia or stress. Erythromelalgia can occur either as a primary or secondary disorder (i.e. a disorder in and of itself or a symptom of another condition). Secondary erythromelalgia can result from small fiber peripheral neuropathy of any cause, essential thrombocytosis, hypercholesterolemia, mushroom or mercury poisoning, and some autoimmune disorders. Primary erythromelalgia is caused by mutation of the voltage-gated sodium channel α-subunit gene SCN9A.
In 2004 Erythromelalgia became the first human disorder in which it has been possible to associate an ion channel mutation with chronic neuropathic pain;[2] this became possible when a Yale neurologist spotted a Beijing geneticists team paper in the Journal of Medical Genetics titled "Mutations in SCN9A, Encoding a Sodium Channel Alpha Subunit, in Patients With Primary Erythromelalgia"; a connection was made that this sodium channel mutation was expressed primarily in peripheral pain sensing neurons.[3] Conversely, in December 2006 a University of Cambridge team reported an SCN9A mutation that created a complete "lack of" pain sensation in the family of a Pakistan street performer. He felt no pain, walked on hot coals and stabbed himself to entertain crowds.
Contents
Classification
Primary erythromelalgia may be classified as either familial or sporadic, with the familial form inherited in an autosomal dominant manner. Both of these may be further classified as either juvenile or adult onset. Juvenile onset occurs prior to age 20 and frequently prior to age 10. While the genetic cause of the juvenile and sporadic adult onset forms is often known, this is not the case for the adult onset familial form.[4]
Incidence
Recent research in the U.S. found the incidence of EM (the number of people a year diagnosed with EM) to be 1.3 per 100,000. The rate for women was higher — 2.0 per 100,000 per year — than men, which was just 0.6. The median age at diagnosis was 61. These rates were five times higher than those estimated by an earlier Norwegian study — the only other known research describing EM incidence. Approximately five percent of those with EM have the autosomal dominant (Primary-Inherited) form of the disease.[5]
Symptoms and signs
The most prominent symptoms of erythromelalgia are episodes of erythema, swelling, a painful deep-aching of the soft tissue (usually either radiating or shooting) and tenderness, along with a painful burning sensation primarily in the extremities. These symptoms are often symmetric and affect the lower extremities more frequently than the upper extremities. Symptoms may also affect the ears and face. For secondary erythromelalgia, attacks typically precede and are precipitated by the underlying primary condition. For primary erythromelalgia, attacks can last from an hour to months at a time and occur infrequently to frequently with multiple times daily. Common triggers for these episodes are exertion, heating of the affected extremities, and alcohol or caffeine consumption, and any pressure applied to the limbs. In some patients sugar and even melon consumption have also been known to provoke attacks. Many of those with primary erythromelalgia avoid wearing shoes or socks as the heat this generates is known to produce erythromelalgia attacks.[4] Raynaud's often coexists in patients with Erythromelalgia[6]
Cause
In general, erythromelalgia seems to consist of neuropathological and microvascular alterations. How this occurs in secondary erythromelalgia is poorly understood and may be specific to the underlying primary condition. Primary conditions that have been shown to elicit erythromelalgia are listed in diagnosis, below.[4]
Primary erythromelalgia is a better understood autosomal dominant disorder. The neuropathological symptoms of primary erythromelalgia arise from hyperexcitability of C-fibers in the dorsal root ganglion. Specifically, nociceptors (neurons responsible for the sensation and conduction of painful stimuli) appear to be the primarily affect neurons in these fibers. This hyperexcitability results in the severe burning pain experienced by patients. While the neuropathological symptoms are a result of hyperexcitability, microvascular alterations in erythromelalgia are due to hypoexcitability. The sympathetic nervous system controls cutaneous vascular tone and altered response of this system to stimuli such as heat likely results in the observed microvascular symptoms. In both cases, these changes in excitability are typically due to mutation of the sodium channel NaV1.7. These differences in excitability alterations between the sympathetic nervous system and nociceptors is due to different expression of sodium channels other than NaV1.7 in them.[4]
Side effect of medication
Several medications including ergot derivatives like bromocriptine and pergolide, verapamil, and nifedipine have been associated with medication-induced erythromelalgia.
Mushroom poisoning
The consumption of two species of related fungi, Clitocybe acromelalga from Japan,[7] and Clitocybe amoenolens from France,[8] has led to several cases of mushroom-induced erythromelalgia which lasted from 8 days to 5 months.[9]
Pathophysiology
N.B. This section pertains solely to primary erythromelalgia as the secondary form is too poorly understood.
There are 10 known mutations in the voltage-gated sodium channel α-subunit NaV1.7 encoding gene, SCN9A. This channel is expressed primarily in nociceptors of the dorsal root ganglion and the sympathetic ganglion neurons. 9 of these mutations have received further study and they have all shown to result in similar biophysical alterations, Table 1. As can be seen from table 1, the primary effect of erythromelalgia mutations is NaV1.7 channels that activate at more hyperpolarized potentials. NaV1.7 channels act largely as threshold sensors and initiate action potentials. Consequently, this shift in their activation profile results in channels that open closer to the resting membrane potential. In many mutations, this shift of activation is accompanied by shifts in the voltage sensitivity of fast and/or slow inactivation, often in the depolarized direction. This results in channels that are open for a longer of period of time, producing larger and more prolonged changes in membrane potential.
Some of these mutant channels have been expressed in dorsal root ganglion (DRG) or sympathetic neurons. In DRG neurons expressing the F1449V mutation, a lower threshold is required for action potential creation (93.1 ± 12.0 pA) than those expressing wild-type channels (124.1 ± 7.4 pA). Furthermore, while DRG neurons expressing wild-type channels only respond with a few action potentials, those expressing F1449V channels respond with a high-frequency train of action potentials.[10] There is a similar effect in DRG neurons expressing the L858H and A863P mutants. Here, there is also a notable change in resting membrane potential, being depolarized by 4-7 mV versus wild-type channel expressing cells.[11][12] The situation is different, however, in sympathetic neurons expressing the L858H mutation. While L858H expressing sympathetic ganglion are depolarized ~5mV relative to wild-type expressing neurons, their threshold for action potential initian is notably higher. Furthermore, while current injection of 40pA for 950ms provokes an average of 6 action potentials in sympathetic neurons expressing wild-type channels this stimulation evokes only approximately 2 action potentials with reduced overshoots in sympathetic neurons expressing L858H mutant channels. Further investigation has demonstrated that the differences in response between DRG and sympathetic neurons is due to expression of NaV1.8 in the former. Consequently, expression of NaV1.8 channels in sympathetic neurons also expressing L858H mutant NaV1.7 results in neurons with a depolarized resting membrane potential that nevertheless have a normal action potential threshold and overshoot.[11]
An effective, though not recommended, treatment for erythromelalgia symptoms is cooling of the affected area. Activation of wild-type channels is unaffected by cooling. L858F mutant channels, however, are activated at more depolarized potentials when cooled than at normal body temperature. At 16°C the activation V½ of the mutant channel is only 4.6mV more hyperpolarized that wild-type versus 9.6mV more hyperpolarized at 35°C. Fast inactivation is affected in a similar manner in both wild-type and L858F mutant channel and is, thus, unlikely to contribute to symptom resolution due to cooling. While such cooling is unlikely to affect neuronal cell bodies, axons and termini express NaV1.7 and are present in the skin.[13]
Table 1. Summary of mutations NaV1.7 associated with primary erythromelalgia Mutation Region Shift of activation V½ Shift of inactivation (fast and/or slow) V½ Other effects References I136V D1S1 [14] F216S D1S4 Hyperpolarized Hyperpolarized Faster entry into fast-inactivation [15][16][17] S241T D1S4-5 Hyperpolarized Hyperpolarized [18][19] N395K D1S6 Hyperpolarized Depolarized Creation of a large window current, decreased lidocaine sensitivity [15][17] I848T D2S4-5 Hyperpolarized Slowed deactivation and inactivation [15][3][20] L858F D2S4-5 Hyperpolarized Depolarized Slowed deactivation, faster recovery from inactivation, cooling depolarizes activation and hyperpolarizes inactivation V½ [13][15][21] L858H D2S4-5 Hyperpolarized Slowed deactivation, enhanced slow inactivation, [11][15][3][20] A863P D2S5 Hyperpolarized Depolarized Creation of a window current, slowed deactivation [12] F1449V D3-4 Hyperpolarized [10] Region nomenclature: DA-B, linker between domains A and B; DASB, transmembrane segment B in domain A; and DASB-C, the linker between transmembrane segments B and C in domain A. Diagnosis
See also: Burning feet syndromeErythromelalgia is a difficult condition to diagnose as there are no specific tests available. To get a diagnosis can take many months and the patient will often have seen 6 or 7 specialists before finding out what is wrong with them.[citation needed] Once it has been established that it is not secondary erythromelalgia — see below — then a programme of management can be put in place. Some diseases present with symptoms similar to erythromelalgia. Complex regional pain syndrome (CRPS), for instance, presents with severe burning pain and redness except these symptoms are often unilateral (versus symmetric) and may be proximal instead of purely or primarily distal. Furthermore, attacks triggered by heat and resolved by cooling are less common with CRPS.
Erythromelalgia is sometimes caused by other disorders. A partial list of diseases known to precipitate erythromelalgia is below.[4]
-
- Myeloproliferative disease
- Hypercholesterolemia
- Autoimmune disorder
- Small fiber peripheral neuropathy
- Fabry's disease
- Mercury poisoning
- Mushroom poisoning
- Sciatica
- Some medications, such as bromocriptine, pergolide, verapamil and ticlopidine
Treatment/Management
For secondary erythromelalgia, treatment of the underlying primary disorder is the most primary method of treatment, though aspirin may reduce symptoms of erythromelalgia. Mechanical cooling of the limbs by elevating them, placing in cool water, or managing the ambient environment frequently is often necessary constantly as flares occur due to sympathetic autonomic dysfunction of the capillaries. The pain that accompanies it is severe and treated separately (the pain is similar to CRPS, phantom limb or thalamic pain syndrome).
Primary erythromelalgia management is symptomatic, i.e. treating painful symptoms only. Specific management tactics include avoidance of attack triggers such as: heat, change in temperature, exercise or over exertion, alcohol and spicy foods. This list is by no means comprehensive as there are many triggers to set off a 'flaring' episode. Whist a cool environment is helpful in keeping the symptoms in control, the use of cold water baths is discouraged as such since erythromelalgia sufferers pain is extreme. In pursuit of added relief sufferers can inadvertently cause tissue damage or death, i.e., necrosis.[citation needed] One clinical study has demonstrated the efficacy of IV lidocaine or oral mexilitine, though it should be noted that differences between the primary and secondary forms was not studied. Another trial has shown promise for misoprostol, while other have shown that gabapentin, venlafaxine, and oral magnesium may also be effective.[4] Anecdotal evidence shows that a combination of drugs such as duloxetine and pregabalin is an effective way of reducing the symptoms of erythromelalgia in conjunction with analgesia.[citation needed] Most people with erythromelalgia do not go into remission and the symptoms are ever present at some level. Again, anecdotally, many of those suffering with EM are prescribed ketamine topical creams as a way of managing pain on a long term basis.[22]
Living with erythromelalgia can result in a deterioration in quality of life resulting in the inability to function in a work place, lack of mobility, depression and is socially alienating; greater education of medical practitioners is needed. As with many rare diseases, many people with EM end up taking years to get a diagnosis and to receive appropriate treatment.
Research into the genetic mutations continues but there is a paucity of clinical studies focusing on living with erythromelalgia. There is much urgency within pharmaceutical companies to provide a solution to those who suffer with pain such as that with erythromelalgia.
External links
- The Erythromelalgia Association
- Hisama FM, Dib-Hajj SD, Waxman SG (September 2008). "SCN9A-Related Inherited Erythromelalgia". In Pagon RA, Bird TD, Dolan CR, et al. GeneReviews. PMID 20301342. NBK1163. http://www.ncbi.nlm.nih.gov/books/NBK1163/.
Footnotes
- ^ James, William D.; Berger, Timothy G.; et al. (2006). Andrews' Diseases of the Skin: clinical Dermatology. Saunders Elsevier. p. 816. ISBN 0-7216-2921-0.
- ^ Waxman, Stephan G.; Dib-Hajj, Sulayman D. (June 2005). "Erythromelalgia: A hereditary pain syndrome enters the molecular era". Annals of Neurology 57 (6): 785–8. doi:10.1002/ana.20511. PMID 15929046.
- ^ a b c Yang Y, Wang Y, Li S, et al. (2004). "Mutations in SCN9A, encoding a sodium channel alpha subunit, in patients with primary erythermalgia". J. Med. Genet. 41 (3): 171–4. doi:10.1136/jmg.2003.012153. PMC 1735695. PMID 14985375. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=1735695.
- ^ a b c d e f Novella SP, Hisama FM, Dib-Hajj SD, Waxman SG (2007). "A case of inherited erythromelalgia". Nature clinical practice. Neurology 3 (4): 229–34. doi:10.1038/ncpneuro0425. PMID 17410110.
- ^ Reed KB, Davis MD (January 2009). "Incidence of erythromelalgia: a population-based study in Olmsted County, Minnesota". J Eur Acad Dermatol Venereol 23 (1): 13–5. doi:10.1111/j.1468-3083.2008.02938.x. PMC 2771547. PMID 18713229. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2771547.
- ^ Berlin AL, Pehr K (March 2004). "Coexistence of erythromelalgia and Raynaud's phenomenon". J. Am. Acad. Dermatol. 50 (3): 456–60. doi:10.1016/S0190-9622(03)02121-2. PMID 14988692.
- ^ Ichimura, J (1918). "A new poisonous mushroom". Bot Gaz (Tokyo) 65: 10911.
- ^ Saviuc PF, Danel VC, Moreau PA, Guez DR, Claustre AM, Carpentier PH, Mallaret MP, Ducluzeau R (2001). "Erythromelalgia and mushroom poisoning". J. Toxicol Clin Toxicol 39 (4): 403–07. doi:10.1081/CLT-100105162.
- ^ Diaz, James H. (February 2005). "Syndromic diagnosis and management of confirmed mushroom poisonings". Critical Care Medicine 33 (2): 427–36. doi:10.1097/01.CCM.0000153531.69448.49. PMID 15699849.
- ^ a b Dib-Hajj SD, Rush AM, Cummins TR, et al. (2005). "Gain-of-function mutation in Nav1.7 in familial erythromelalgia induces bursting of sensory neurons". Brain 128 (Pt 8): 1847–54. doi:10.1093/brain/awh514. PMID 15958509.
- ^ a b c Rush AM, Dib-Hajj SD, Liu S, Cummins TR, Black JA, Waxman SG (2006). "A single sodium channel mutation produces hyper- or hypoexcitability in different types of neurons". Proc. Natl. Acad. Sci. U.S.A. 103 (21): 8245–50. doi:10.1073/pnas.0602813103. PMC 1472458. PMID 16702558. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=1472458.
- ^ a b Harty TP, Dib-Hajj SD, Tyrrell L, et al. (2006). "Na(V)1.7 mutant A863P in erythromelalgia: effects of altered activation and steady-state inactivation on excitability of nociceptive dorsal root ganglion neurons". J. Neurosci. 26 (48): 12566–75. doi:10.1523/JNEUROSCI.3424-06.2006. PMID 17135418.
- ^ a b Han C, Lampert A, Rush AM, et al. (2007). "Temperature dependence of erythromelalgia mutation L858F in sodium channel Nav1.7". Molecular pain 3: 3. doi:10.1186/1744-8069-3-3. PMC 1781932. PMID 17239250. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=1781932.
- ^ Lee MJ, Yu HS, Hsieh ST, Stephenson DA, Lu CJ, Yang CC (2007). "Characterization of a familial case with primary erythromelalgia from Taiwan". J. Neurol. 254 (2): 210–4. doi:10.1007/s00415-006-0328-3. PMID 17294067.
- ^ a b c d e Drenth JP, te Morsche RH, Guillet G, Taieb A, Kirby RL, Jansen JB (2005). "SCN9A mutations define primary erythermalgia as a neuropathic disorder of voltage gated sodium channels". J. Invest. Dermatol. 124 (6): 1333–8. doi:10.1111/j.0022-202X.2005.23737.x. PMID 15955112.
- ^ Choi JS, Dib-Hajj SD, Waxman SG (2006). "Inherited erythermalgia: limb pain from an S4 charge-neutral Na channelopathy". Neurology 67 (9): 1563–7. doi:10.1212/01.wnl.0000231514.33603.1e. PMID 16988069.
- ^ a b Sheets PL, Jackson JO, Waxman SG, Dib-Hajj SD, Cummins TR (2007). "A Nav1.7 channel mutation associated with hereditary erythromelalgia contributes to neuronal hyperexcitability and displays reduced lidocaine sensitivity". J. Physiol. (Lond.) 581 (Pt 3): 1019–31. doi:10.1113/jphysiol.2006.127027. PMC 2170829. PMID 17430993. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2170829.
- ^ Michiels JJ, te Morsche RH, Jansen JB, Drenth JP (2005). "Autosomal dominant erythermalgia associated with a novel mutation in the voltage-gated sodium channel alpha subunit Nav1.7". Arch. Neurol. 62 (10): 1587–90. doi:10.1001/archneur.62.10.1587. PMID 16216943.
- ^ Lampert A, Dib-Hajj SD, Tyrrell L, Waxman SG (2006). "Size matters: Erythromelalgia mutation S241T in Nav1.7 alters channel gating". J. Biol. Chem. 281 (47): 36029–35. doi:10.1074/jbc.M607637200. PMID 17008310.
- ^ a b Cummins TR, Dib-Hajj SD, Waxman SG (2004). "Electrophysiological properties of mutant Nav1.7 sodium channels in a painful inherited neuropathy". J. Neurosci. 24 (38): 8232–6. doi:10.1523/JNEUROSCI.2695-04.2004. PMID 15385606.
- ^ Han C, Rush AM, Dib-Hajj SD, et al. (2006). "Sporadic onset of erythermalgia: a gain-of-function mutation in Nav1.7". Ann. Neurol. 59 (3): 553–8. doi:10.1002/ana.20776. PMID 16392115.
- ^ Sandroni P, Davis MD (March 2006). "Combination gel of 1% amitriptyline and 0.5% ketamine to treat refractory erythromelalgia pain: a new treatment option?". Arch Dermatol 142 (3): 283–6. doi:10.1001/archderm.142.3.283. PMID 16549702. http://archderm.ama-assn.org/cgi/pmidlookup?view=long&pmid=16549702.
Genetic disorder, membrane: Channelopathy Calcium channel CACNA1A (Familial hemiplegic migraine 1, Episodic ataxia 2, Spinocerebellar ataxia type-6) · CACNA1C (Timothy syndrome, Brugada syndrome 3, Long QT syndrome 8) · CACNA1F (Ocular albinism 2, CSNB2A) · CACNA1S (Hypokalemic periodic paralysis 1, Thyrotoxic periodic paralysis 1) · CACNB2 (Brugada syndrome 4)Ligand gatedSodium channel Voltage-gatedSCN1A (Familial hemiplegic migraine 3, GEFS+ 2, Febrile seizure 3A) · SCN1B (Brugada syndrome 6, GEFS+ 1) · SCN4A (Hypokalemic periodic paralysis 2, Hyperkalemic periodic paralysis, Paramyotonia congenita, Potassium-aggravated myotonia) · SCN4B (Long QT syndrome 10) · SCN5A (Brugada syndrome 1, Long QT syndrome 3) · SCN9A (Erythromelalgia, Febrile seizure 3B, Paroxysmal extreme pain disorder, Congenital insensitivity to pain)Potassium channel KCNA1 (Episodic ataxia 1) · KCNA5 (Familial atrial fibrillation 7) · KCNC3 (Spinocerebellar ataxia type-13) · KCNE1 (Jervell and Lange-Nielsen syndrome, Long QT syndrome 5) · KCNE2 (Long QT syndrome 6) · KCNE3 (Brugada syndrome 5) · KCNH2 (Short QT syndrome) · KCNQ1 (Jervell and Lange-Nielsen syndrome, Romano-Ward syndrome, Short QT syndrome, Long QT syndrome 1, Familial atrial fibrillation 3) · KCNQ2 (BFNS1}KCNJ1 (Bartter syndrome 2) · KCNJ2 (Andersen-Tawil syndrome, Long QT syndrome 7, Short QT syndrome) · KCNJ11 (TNDM3) · KCNJ18 (Thyrotoxic periodic paralysis 2)Chloride channel TRP channel Connexin GJA1 (Oculodentodigital dysplasia, Hallermann–Streiff syndrome, Hypoplastic left heart syndrome) · GJB1 (Charcot–Marie–Tooth disease X1) · GJB2 (Keratitis–ichthyosis–deafness syndrome, Ichthyosis hystrix, Bart–Pumphrey syndrome, Vohwinkel syndrome) · GJB3/GJB4 (Erythrokeratodermia variabilis, Progressive symmetric erythrokeratodermia) · GJB6 (Clouston's hidrotic ectodermal dysplasia)Porin Categories:- Channelopathy
- Neurological disorders
- Vascular-related cutaneous conditions
- Diseases of arteries, arterioles and capillaries
-
Wikimedia Foundation. 2010.
