- Low molecular weight heparin
-
In medicine, low-molecular-weight heparin (LMWH) is a class of medication used as an anticoagulant in diseases that feature thrombosis, as well as for prophylaxis in situations that lead to a high risk of thrombosis.[1]
Thrombotic disease or thrombosis is the formation of a clot within a blood vessel which interferes with the blood supply to tissues and causes problems such as deep vein thrombosis, pulmonary embolism when it is located in the veins, or heart attacks and strokes when located in the arteries.
Heparin is a naturally occurring polysaccharide that inhibits coagulation, the process whereby thrombosis occurs (see Heparin: Mechanisms of action). Natural heparin consists of molecular chains of varying lengths, or molecular weights. Chains of molecular weight from 5000 to over 40,000 Daltons, making up polydisperse pharmaceutical-grade heparin.[2]
Heparin derived from natural sources, mainly porcine intestine or bovine lung, can be administered therapeutically to prevent thrombosis. However, the effects of natural, or unfractionated heparin can be difficult to predict. After a standard dose of unfractionated heparin, coagulation parameters must be monitored very closely to prevent over- or under-anticoagulation.
Low-molecular-weight heparins (LMWHs), in contrast, consist of only short chains of polysaccharide. LMWHs are defined as heparin salts having an average molecular weight of less than 8000 Da and for which at least 60% of all chains have a molecular weight less than 8000 Da. These are obtained by various methods of fractionation or depolymerisation of polymeric heparin.
Contents
Anti-factor Xa activity
Coagulation cascade is a normal physiological process which aims at preventing significant blood loss or hemorrhage following vascular injury. Unfortunately, there are times when a blood clot (thrombus) will form when it is not needed. For instance, some high risk conditions such as acute medical illness prolonged immobilization, surgery, or cancer can increase the risk of developing a blood clot which can potentially lead to significant consequences.
The coagulation cascade consists of a series of steps in which a protease cleaves and subsequently activates the next protease in the sequence[2]. Since each protease can activate several molecules of the next protease in the series, this biological cascade is amplified. The final result of these reactions is to convert fibrinogen, a soluble protein, to insoluble threads of fibrin. Together with platelets, the fibrin threads form a stable blood clot.
Antithrombin (AT), a serine protease inhibitor, is the major plasma inhibitor of coagulation proteases[3]. LMWHs inhibit the coagulation process through binding to AT via a pentasaccharide sequence. This binding leads to a conformational change of AT which accelerates its inhibition of thrombin (factor IIa) and activated factor X (factor Xa). Once dissociated, the LMWH is free to bind to another antithrombin molecule and subsequently inhibit more thrombin.
The effects of LMWHs cannot be acceptably measured using the partial thromboplastin time (PTT) or activated clotting time (ACT) tests.[4] Rather, LMWH therapy is monitored by the anti-factor Xa assay, measuring anti-factor Xa activity. The methodology of an anti-factor Xa assay is that patient plasma is added to a known amount of excess factor Xa and excess antithrombin. If heparin or LMWH is present in the patient plasma, it will bind to antithrombin and form a complex with factor Xa, inhibiting it.[5] The amount of residual factor Xa is inversely proportional to the amount of heparin/LMWH in the plasma. The amount of residual factor Xa is detected by adding a chromogenic substrate that mimics the natural substrate of factor Xa, making residual factor Xa cleave it, releasing a colored compound that can be detected by a spectrophotometer.[5] Antithrombin deficiencies in the patient do not affect the assay, because excess amounts of antithrombin is provided in the reaction.[5] Results are given in anticoagulant concentration in units/mL of antifactor Xa, such that high values indicate high levels of anticoagulation and low values indicate low levels of anticoagulation.[5]
LMWHs have a potency of greater than 70 units/mg of anti-factor Xa activity and a ratio of anti-factor Xa activity to anti-thrombin activity of >1.5.[6] (see table 1)
LMWH Average molecular weight Ratio anti-Xa/anti-IIa activity Bemiparin 3600 9.7 Certoparin 5400 2.4 Dalteparin 6000 2.5 Enoxaparin 4500 3.9 Nadroparin 4300 3.3 Parnaparin 5000 2.3 Reviparin 4400 4.2 Tinzaparin 6500 1.6 Table 1 Molecular weight (MW) data and anticoagulant activities of currently available LMWH products. Adapted from Gray E et al. 2008[7].
Manufacturing Process
Various methods of heparin depolymerisation are used in the manufacture of low-molecular-weight heparin.[2] These are listed below:
- Oxidative depolymerisation with hydrogen peroxide. Used in the manufacture of ardeparin (Normiflo)
- Deaminative cleavage with isoamyl nitrite. Used in the manufacture of certoparin (Sandoparin)
- Alkaline beta-eliminative cleavage of the benzyl ester of heparin. Used in the manufacture of enoxaparin (Lovenox and Clexane)
- Oxidative depolymerisation with Cu2+ and hydrogen peroxide. Used in the manufacture of parnaparin (Fluxum)
- Beta-eliminative cleavage by the heparinase enzyme. Used in the manufacture of tinzaparin (Innohep and Logiparin)
- Deaminative cleavage with nitrous acid. Used in the manufacture of dalteparin (Fragmin), reviparin (Clivarin) and nadroparin (Fraxiparin)
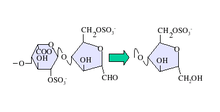
Deaminative cleavage with nitrous acid results in the formation of an unnatural anhydromannose residue at the reducing terminal of the oligosaccharides produced. This can subsequently be converted to anhydromannitol using a suitable reducing agent as shown in figure 1.
 Figure 2: UA(2S)-GlcNS(6S)
Figure 2: UA(2S)-GlcNS(6S)
Likewise both chemical and enzymatic beta-elimination result in the formation of an unnatural unsaturated uronate residue(UA) at the non-reducing terminal, as shown in figure 2.
Differences between low molecular weight heparin products
Comparisons between LMWHs prepared by similar processes vary. For example, a comparison of Dalteparin and Nadroparin suggests they are more similar than products produced by different processes. However, comparison of enoxaparin and tinzaparin shows they are very different from each other with respect to chemical, physical, and biological properties.
As might be expected, products prepared by distinctly different processes are dissimilar in physical, chemical, and biological properties[2][8]. Hence a slight change in the depolymerisation process could result into substantial variation of the structure or composition of a given LMWH.
Therefore for every LMWH, a strictly defined depolymerisation procedure is needed to guarantee the sameness of the final LMWH product and the predictability of clinical outcomes. LMWHs, as biological origin products, rely on stringent manufacturing procedures to guarantee the absence of biological or chemical contamination. It is therefore critical to adopt stringent manufacturing practices, through rigorous quality assurance steps, to ensure the highest quality of the produced LMWHs and to guarantee patient safety. These quality assurance steps, to be effective, need to be implemented from the raw material (crude heparin) collection to the final LMWH product.
Due to these identified and potential differences, several organizations, including the United States Food and Drug Administration, the European Medicines Agency, and the World Health Organization, regard LMWHs as individual products that should not be considered as clinically equivalent, as they differ in many crucial aspects such as molecular, structural, physiochemical and biological[9][10][11]. According to international guidelines, the choice of an individual LMWH should be based on its proven clinical safety and efficacy for each indication[12].
Differences from unfractionated heparin
Its differences with heparin (i.e. "unfractioned heparin") include:
- Average molecular weight: heparin is about 15 kDa and LMWH is about 4.5 kDa.[13]
- Less frequent subcutaneous dosing than for heparin for postoperative prophylaxis of venous thromboembolism.
- Once or twice daily subcutaneous injection for treatment of venous thromboembolism and in unstable angina instead of intravenous infusion of high dose heparin.
- No need for monitoring of the APTT coagulation parameter as required for high dose heparin.[14]
- Possibly a smaller risk of bleeding.
- Smaller risk of osteoporosis in long-term use.
- Smaller risk of heparin-induced thrombocytopenia, a potential side effect of heparin.
- The anticoagulant effects of heparin are typically reversible with protamine sulfate, while protamine's effect on LMWH is limited.
- Has less of an effect on thrombin compared to heparin, but about the same effect on Factor Xa.
Clinical uses
Because it can be given subcutaneously and does not require APTT monitoring, LMWH permits outpatient treatment of conditions such as deep vein thrombosis or pulmonary embolism that previously mandated inpatient hospitalization for unfractionated heparin administration.
Because LMWH has more predictable pharmacokinetics and anticoagulant effect, LMWH is recommended over unfractionated heparin for patients with massive pulmonary embolism,[15] and for initial treatment of deep vein thrombosis.[16] Prophylactic treatment of hospitalized medical patients with LMWH and similar anticoagulants results in a 53% reduction of risk for symptomatic deep vein thrombosis.[17]
More recently these agents have been evaluated as anticoagulants in acute coronary syndrome (ACS) managed by percutaneous intervention (PCI)[18][19].
The use of LMWH needs to be monitored closely in patients at extremes of weight or in-patients with renal dysfunction. An anti-factor Xa activity may be useful for monitoring anticoagulation. Given its renal clearance, LMWH may not be feasible in patients that have end-stage renal disease.
Use in venothromboembolic disease associated with cancer
The CLOT study, published in 2003, showed that, in patients with malignancy and acute venous thromboembolism, dalteparin was more effective than coumadin in reducing the risk of recurrent embolic events.[20] Use of LMWH in cancer patients for at least the first 3 to 6 months of long-term treatment is recommended in numerous guidelines and is now regarded as a standard of care.[21]
LMWH antidote
In clinical situations in which the antithrombotic effect of LMWHs needs to be neutralized, protamine is used to neutralize heparin by binding to it.[22]Studies in animals and in vitro studies have demonstrated that protamine neutralizes the antithrombin activity of LMWHs, normalizing the aPTT and thrombin time. However, protamine appears to only partially neutralize the anti-factor Xa activity of LMWH. Because the molecular weight of heparin impacts on its interaction with protamine, it is likely that the lack of complete neutralization of anti-factor Xa is due to a reduced protamine binding to the LMWHs moieties in the preparation. Protamine is a medicine that requires a high level of caution when being used.
Contraindications
The use of LMWHs should be avoided in patients with known allergies to LMWHs, heparin, sulfites or benzyl alcohol, in patients with active major bleeding, or patients with a history of heparin-induced low blood platelet count (also known as heparin-induced thrombocytopenia or HIT). High treatment doses are counter indicated in acute bleedings such as cerebral or gastrointestinal haemorrhage.
Precautions in use
LMWHs should be used with extreme cautions in patients undergoing any procedure involving spinal anaesthesia/puncture, in conditions with increased risk of bleeding or in patients with a history of heparin-induced thrombocytopenia.
Side effects
The most common side-effects include bleeding, which could be severe or even fatal, allergic reactions, injection site reactions, and increases in liver enzyme tests, usually without symptoms[23]. The use of heparin and LMWHs can sometimes be complicated by a decrease in platelet count, a complication known as Heparin Induced Thrombocytopenia.13 Two forms have been described: a clinically benign, non-immune and reversible form (Type I) and a rare, more serious immune-mediated form or Type II. HIT Type II is caused by the formation of auto antibodies that recognize complexes between heparin and platelet factor 4 (PF4) and is therefore associated with a substantial risk of thrombotic complications. The incidence is difficult to estimate but may reach up to 5% of patients treated with UFH or about 1% with LMWH[24].
LMWHs Biosimilars
The patents of LMWHs are expiring. Therefore, copies of LMWHs are being produced by several companies; these copies of LMWHs are named biosimilars or generics depending on the regulatory agencies rules. The first ‘generic version’ of a LMWH was approved by the Food and Drug Administration end of July 2010. FDA has used 5 analytical and pharmacological criteria to establish the sameness of a generic version of enoxaparin, without clinical studies in patients [25].
The European Medicines Agency considers LMWHs as biological products in nature consisting of not fully characterised polysaccharide mixtures. Therefore EMA requires that the efficacy and safety of a biosimilar LMWH candidate has to be established in a clinical trial with patients at high risk for thromboembolism.
See also
References
- ^ Weitz JI; Weitz, Jeffrey I. (1997). "Low-molecular-weight heparins". N Engl J Med 337 (10): 688–98. doi:10.1056/NEJM199709043371007. PMID 9278467.
- ^ a b c d Linhardt, R.J. Gunay, N. S. (1999). "Production and chemical processing of low molecular weight heparins". Sem. Thromb. Hem. 25 (3): 5–16.
- ^ Jeske W, Walenga J, Fareed J. Differentiating between the Low-Molecular-Weight-Heparin used for VTE treatment and prophylaxis. Thromb Clin. 2008;2(3)
- ^ enotes.com > Encyclopedia of Nursing & Allied Health > Coagulation Tests Retrieved on April 5, 2010
- ^ a b c d massgeneral.org > Heparin Antifactor Xa Assay Page Updated: September 18, 2009
- ^ European Pharmacopedia Commission (1991). Pharmeuropa 3: 161–165.
- ^ Gray E, Mulloy B, Barrowcliffe TW. Heparin and low-molecular-weight-heparin. Thromb Haemost 2008; 99: 807–818.
- ^ Jeske W, Walenga J, Fareed J. Differentiating between the Low-Molecular-Weight-Heparin used for VTE treatment and prophylaxis. Thromb Clin. 2008;2(3)
- ^ WHO Working Group on Biological Standardization of Unfractionated Heparin, WHO Headquarters, Geneva, Switzerland, 7-8 September, 1999
- ^ EMA/CHMP/BMWP/118264/2007. Guideline on non-clinical andclinical development of similar biological medicinal products containing Low-molecular-weight-heparins. March 2009.
- ^ The US Food and Drug Administration (FDA) alert. JAMA. 1993;270:1672.
- ^ Nicolaides AN. et al. Prevention and treatment of venous thromboembolism. International Consensus Statement (ICS). Guidelines according to scientific evidence. Int Angiol. 2006;25:101-61
- ^ Michael D Randall; Karen E Neil (2004). Disease management. 2nd ed. London: Pharmaceutical Press. 186.
- ^ http://chestjournal.chestpubs.org/content/119/1_suppl/64S.full
- ^ Hull RD (2008). "Treatment of pulmonary embolism: The use of low-molecular-weight heparin in the inpatient and outpatient settings". Thrombosis and Haemostasis 99 (3): 502–510. doi:10.1160/TH07-08-0500. PMID 18327398.
- ^ Snow V, Qaseem A, Barry P, Hornbake ER, Rodnick JE, Tobolic T, Ireland B, Segal JB, Bass EB, Weiss KB, Green L, Owens DK; American College of Physicians; American Academy of Family Physicians Panel on Deep Venous Thrombosis/Pulmonary Embolism (2007). "Management of venous thromboembolism: a clinical practice guideline from the American College of Physicians and the American Academy of Family Physicians". Annals of Internal Medicine 146 (3): 204–210. PMID 17261857. http://www.annals.org/cgi/content/full/146/3/204.
- ^ Douketis JD, Moinuddin I (2008). "Prophylaxis against venous thromboembolism in hospitalized medical patients: an evidence-based and practical approach". Polskie Archiwum Medycyny Wewnętrznej 118 (4): 209–215. PMID 18575420. http://tip.org.pl/pamw/issue/article/164.html.
- ^ Montalescot G, White HD, Gallo R, et al. Enoxaparin in Primary and Facilitated Percutaneous Coronary Intervention. JACC Cardiovasc Interv. 2010 Feb;3(2):203-12
- ^ Dumaine R et al. Intravenous Low-Molecular-Weight Heparins Compared With Unfractionated Heparin in Percutaneous Coronary Intervention. Arch Intern Med. 2007;167(22):2423-2430
- ^ Lee AY, Levine MN, Baker RI, Bowden C, Kakkar AK, Prins M, Rickles FR, Julian JA, Haley S, Kovacs MJ, Gent M (2003). "Low-molecular-weight heparin versus a coumadin for the prevention of recurrent venous thromboembolism in patients with cancer". N Engl J Med 349 (2): 146–53. doi:10.1056/NEJMoa025313. PMID 12853587.
- ^ Nishioka J, Goodin S (2007). "Low-molecular-weight heparin in cancer-associated thrombosis: treatment, secondary prevention, and survival". Journal of Oncology Pharmacy Practice 13 (2): 85–97. doi:10.1177/1078155207079169. PMID 17873108.
- ^ Dumaine R et al. Intravenous Low-Molecular-Weight Heparins Compared With Unfractionated Heparin in Percutaneous Coronary Intervention. Arch Intern Med. 2007;167(22):2423-2430
- ^ Nicolaides AN. et al. Prevention and treatment of venous thromboembolism. International Consensus Statement (ICS). Guidelines according to scientific evidence. Int Angiol. 2006;25:101-61.
- ^ Nicolaides AN. et al. Prevention and treatment of venous thromboembolism. International Consensus Statement (ICS). Guidelines according to scientific evidence. Int Angiol. 2006;25:101-61.
- ^ Harenberg J. Overview on guidelines and recommendations for generic low-molecular-weight heparins. Thrombosis Research 127 Suppl. 3 (2011) S100–S104
External links
Categories:- Heparins
Wikimedia Foundation. 2010.